Partnership Principles
Strong partnerships take time and investment because partners may have different priorities. A working partnership requires all parties to value and respect each other. While partnerships can be defined in various ways, below are core practices that support ethical and responsible partnerships, especially when using local data:
Core Practices that Support Ethical and Responsible Partnerships
- Focus on shared priorities (e.g. what are shared goals between partners)
- Discuss and work within scope (e.g. What is realistic to accomplish given timeline, funding, other constraints?)
- Enhance organizational capacities - All parties should be able to do more because of this partnership
- Develop/build on long-term partnerships - These partnerships are often built over years, not months
- Take time to build trust - This is an essential element of a successful partnership
- Facilitate reciprocal learning - Everyone grows in their knowledge
- Adapt interventions/strategies to cultural and local contexts - Meet the needs of the unique community and the people who live there
- Value local knowledge – Members of the community likely know the needs and have ideas for solutions
- Engage or train leaders from communities you are working with
- Provide resources to community partners - Make sure local residents have what they need to fully participate as partners
- Ensure that programs/research projects serve the goals of the communities they are engaging
To build the strongest possible partnerships, all involved parties should work together to share leadership. In a shared leadership model, strong bidirectional trust is built between partners, and final decision making is at the community level. The National Institutes of Health has a detailed report covering the Principles of Community Engagement which can help partnerships move towards shared leadership. In the graphic below you will see the Spectrum of Public Participation, which organizes the core values of community engagement into a diagram to demonstrate the different levels of engagement with partners.
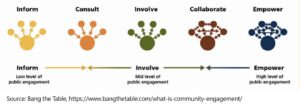
Valuing Everyone at the Table
It can be helpful to reflect on your role and what you can do to better understand other partnership roles. In the dropdown below, please select the statement that feels most true to your role in this work to learn more. Community partners is a broad category and may include non-profits, state and local government organizations, clinics, pharmacies, and more.
Partnering with researchers offers many benefits for community partners. The ways in which a community partner work with a researcher can look different depending on what the researcher studies. A researcher may be able to provide data to a community partner that can be helpful when applying for funding or grants. Researchers may also be able to provide funding to community partners who partner with them on grants. Researchers can also help community partners figure out how to design or modify interventions to make the community healthier. Finally, researchers can help spread the word about the successful work going on in the community through their connections to statewide and national networks. Even if both groups have similar goals, the ways that community partners and researchers go about their work can cause tension. Researchers are generally concerned with collecting and using data, which takes time and effort. They want to use evidence to understand how and why a community becomes more healthy. Community partners, on the other hand, are often focused on meeting the immediate needs of the people that they serve. They have years of experience through living and working in their community. They can feel that they already know what “works” and does not work – no additional evidence required. Community partners should be leaders in the discussion around research to ensure that the community’s needs are being met and that community members are empowered and valued throughout the process. One resource for community partners is the Building Trust Between Minorities and Researchers website provided by the University of Maryland Center for Health Equity. This site has several helpful resources for community partners such as: the Importance of Research and Research, Community and You. For Wisconsin-based community organizations interested in working with a researcher, the following resources may provide a good place to start: Community partners are generally concerned with making a direct impact on their community and are often focused on service provision. They want to make local residents healthier and their neighborhoods stronger. For community partners to value research and evaluation, it must be relevant and useful for their community. Even if both groups have similar goals, the different ways that community partners and researchers go about doing the work can cause tension. Researchers are generally concerned with collecting and using data, which can take time and effort. They want to use evidence to understand how and why a community becomes more healthy. Community partners, on the other hand, are often focused on meeting the immediate needs of the people that they serve. They have years of experience through living and working in their community. They can feel that they already know what “works” and does not work – no additional evidence required. It is important to recognize that some community organizations may have had a history of bad experiences with researchers in which they ended up feeling more used than supported. Many communities, particularly communities of color, may not trust outside researchers. This can be especially true for health researchers due to research abuses of the past, such as the Tuskegee Syphilis Study, as well as ongoing experiences of discrimination in health care settings. To build relationships with community partners, it is helpful to understand community development work. It is important to include community partners as leaders throughout the research process to ensure that the community’s needs are being met and that community members are empowered and valued. Allocating grant funding to community partners is also important. To help bridge gaps between minorities and researchers, the University of Maryland Center for Health Equity's website Building Trust Between Minorities and Researchers was created to help both researchers and communities understand what is needed to build equitable community-academic partnerships. For researchers working in areas associated with clinic and health systems, the following articles offer some examples of what a community-academic partnership can look like: For researchers working in public health, the following articles offer examples of what a partnership can look like in that context: For the Neighborhood Health Partnerships (NHP) program, Navigators are the people or organizations who often work with both community partners and researchers. Navigators can help to build trust and relationships between community partners and researchers. They are often the people who help to explain the needs and wants of the different groups in the partnership. They may be skilled at explaining data in a way that is relevant to communities, or skilled at presenting neighborhood priorities in a way that makes sense to researchers. If you are interested in becoming a navigator contact: nhp@hip.wisc.edu. I am a Community Partner
I am a Researcher
I am a NHP Navigator
Connecting to Community Priorities
 The NHP reports can be used to identify needs, inform processes, identify disparities, and support targeted strategic planning. NHP reports can also be used to measure progress toward desired goals, connect health to policies, target services to populations and for surveillance of community health. Here we provide examples of using the reports to serve community priorities.
The NHP reports can be used to identify needs, inform processes, identify disparities, and support targeted strategic planning. NHP reports can also be used to measure progress toward desired goals, connect health to policies, target services to populations and for surveillance of community health. Here we provide examples of using the reports to serve community priorities.
Examples of communities using local health data:
- Often, communities and community-serving groups have an existing list of priorities, including an action plan. Community efforts may be tied to a county-wide Community Health Needs Assessment (CHNA/CHA) and Community Health Improvement Plan (CHIP). The University of Wisconsin Population Health Institute has compiled CHNA/CHAs and CHIPs from hospitals and health departments across the state for easy access.
- Connecting Community Data for Population Health: Supporting Use of EHR Data for Community Health Assessments.
Ideas on using local health data:
- For communities who are working on identifying a list of priorities, County Health Rankings and Roadmaps has a detailed series of activities that can be used to Assess Needs and Resources. These activities can be used to understand current community strengths, resources, needs, and gaps. This can help community members decide where and how to focus their efforts. The Neighborhood Health Reports can be used in several of these activities.
- Community Tool Box has an Assessing Community Needs and Resources toolkit that highlights strategies that can be used to collect qualitative data from community members.
Once community priorities have been selected, the NHP Program has created a curated list of Ideas for Taking Action connected to the different measures available in the reports.
Creating Strong Community-Academic Partnerships
Each NHP report provides a helpful snapshot of neighborhood health data. However, the reports are just one of the many building blocks that can be used in a community-academic partnership. Many of the most effective projects that have improved community health were built on strong partnerships. Community-academic partnerships, in particular, can be an asset to both local organizations as well as researchers.
| Benefits to Communities | Benefits to Researchers |
|
|
Community-Academic Partnerships and the Reports
The local-level health data contained in the reports allows community practitioners and academic researchers to more precisely pinpoint neighborhoods experiencing health disparities and inequities.
These partnerships can support fresh and innovative interventions built with community wisdom and scientifically supported methods. Community-academic partnerships can also help people understand why a particular intervention was successful in a community and whether that success can be repeated in other communities.
Examples of Using Reports for Partnerships
To see how partnerships are engaged in using NHP data, view the Examples page.

